
Pediatric Advanced Life Support (PALS) focuses on systematic assessment, resuscitation, and stabilization of ill infants and children, utilizing current AHA guidelines.
The PALS Provider Manual is essential preparation, offering comprehensive information before, during, and after the course, including a pre-course assessment.
This course aims to improve pediatric care, equipping healthcare providers with crucial skills for managing emergencies, as outlined in the official PALS PDF.
What is Pediatric Advanced Life Support?
Pediatric Advanced Life Support (PALS) represents a comprehensive approach to managing critically ill infants and children. It extends beyond Basic Life Support (BLS), incorporating advanced resuscitation techniques and pharmacological interventions. The core goal, detailed within the PALS PDF, is to effectively assess and stabilize pediatric patients experiencing life-threatening emergencies.
PALS training emphasizes a systematic approach, utilizing algorithms for bradycardia, tachycardia, and respiratory failure. It’s designed for healthcare professionals needing to respond to pediatric emergencies, providing a standardized framework for optimal care, as outlined in the official PALS Provider Manual.
Importance of PALS Certification
PALS certification is crucial for healthcare providers frequently encountering pediatric emergencies. It demonstrates a commitment to providing the highest standard of care, utilizing evidence-based guidelines detailed in the PALS PDF. Certification ensures proficiency in advanced resuscitation techniques, pharmacological management, and effective team dynamics.
Possessing a current PALS Provider credential often fulfills hospital requirements and enhances professional credibility. The PALS Provider Manual equips practitioners with the knowledge to confidently address critical situations, ultimately improving patient outcomes and reducing morbidity, as per AHA standards.
Target Audience for PALS Training
The Pediatric Advanced Life Support (PALS) course, detailed within the PALS PDF, is designed for a diverse group of healthcare professionals. This includes physicians, nurses, paramedics, respiratory therapists, and other individuals involved in the care of critically ill or injured infants and children.
Anyone who might initiate or direct resuscitation efforts benefits from PALS certification. The PALS Provider Manual caters to those needing comprehensive training in pediatric emergency response, ensuring competency in advanced life support techniques and team leadership skills.

The PALS Provider Manual
The PALS Provider Manual is a required text for the course, providing essential information and resources for healthcare providers preparing for certification.
It includes a full-color laminated reference card and is designed for individual use, aiding in mastering PALS PDF content.
Manual as a Course Requirement
The PALS Provider Manual is absolutely mandatory for all participants enrolled in a Pediatric Advanced Life Support course. It serves as the foundational resource, ensuring a standardized learning experience for every student.
Access to the manual, whether in physical or digital PALS PDF format, is crucial for successful completion of the course and subsequent certification. It’s designed for single-user access, promoting focused study and comprehension of the critical concepts.
Without the manual, students will be unable to fully participate in skills stations or the final exam, highlighting its indispensable role in the PALS learning process.
Content Overview of the PALS Manual
The PALS Provider Manual comprehensively covers essential topics, beginning with an introduction to PALS and the resuscitation team’s dynamics. It details Basic Life Support (BLS) interventions tailored for infants and children, forming the bedrock of pediatric emergency care.
Further sections delve into PALS algorithms for bradycardia, tachycardia, and respiratory failure, alongside detailed guidance on CPR techniques and pharmacological management, all accessible within the PALS PDF.
Post-resuscitation care and specific pediatric emergencies like shock and seizures are also thoroughly addressed, providing a holistic understanding of pediatric critical care.
Features of the PALS Provider Manual (2026 Edition)
The 2026 PALS Provider Manual is meticulously designed for individual use, serving as a mandatory resource for all PALS course participants. It’s presented in full color, enhancing readability and comprehension of complex algorithms and procedures detailed within the PALS PDF.
A key feature is the inclusion of a laminated, full-color PALS Reference Card, providing quick access to critical information during simulations and real-life emergencies. This edition reflects the latest AHA guidelines.
The manual also incorporates a pre-course assessment to gauge existing knowledge.
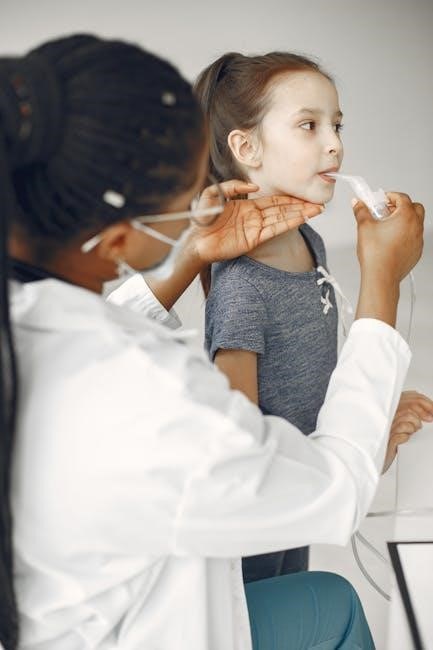
Basic Life Support (BLS) in PALS
PALS builds upon BLS interventions, emphasizing age-specific techniques for infants and children, as detailed in the PALS PDF, to ensure effective resuscitation.
BLS Interventions for Infants
Infant BLS, a foundational component of PALS, requires specific techniques due to their unique anatomy and physiology. The PALS PDF emphasizes checking for responsiveness, activating emergency services, and initiating rescue breaths.
Chest compressions differ, utilizing two fingers or thumbs encircling the chest, compressing approximately one-third the anterior-posterior diameter. Proper head tilt-chin lift is crucial for airway opening, alongside assessing breathing and pulse. The PALS course, guided by the manual, stresses continuous assessment and adaptation of BLS protocols.
BLS Interventions for Children
BLS for children, detailed within the PALS PDF, builds upon infant techniques but adapts to their larger size and developing physiology. Assessment remains paramount – checking responsiveness, activating emergency services, and ensuring airway patency.
Chest compressions utilize the heel of one or two hands, depending on the child’s size, aiming for approximately one-third compression depth. Effective rescue breaths and continuous pulse checks are vital, as highlighted in the PALS course. The manual emphasizes adapting BLS based on the child’s age and condition.
Integration of BLS with Advanced Life Support
The PALS PDF clearly demonstrates how Basic Life Support (BLS) forms the foundation for Advanced Life Support (ALS) in pediatric emergencies. Initial BLS interventions – airway, breathing, circulation – are simultaneously continued while initiating ALS protocols.
ALS builds upon BLS, adding interventions like cardiac monitoring, medication administration, and advanced airway management. The PALS course stresses seamless transition, ensuring no interruption of vital support. Effective teamwork, guided by the PALS algorithms, is crucial for optimal patient outcomes.
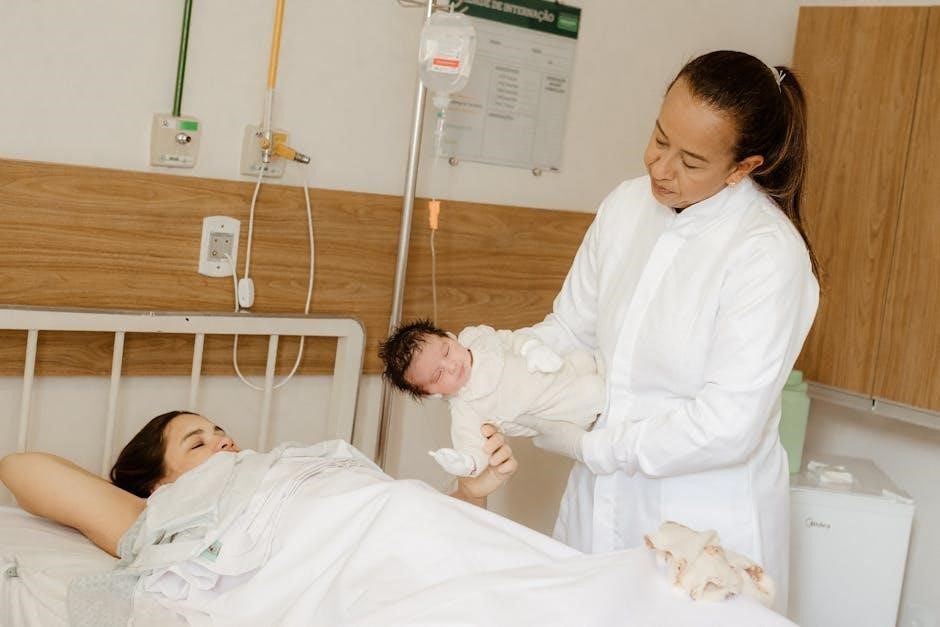
The Resuscitation Team
PALS emphasizes a structured team approach, with clearly defined roles and responsibilities, as detailed in the PALS PDF, for effective pediatric resuscitation.
Successful outcomes depend on strong communication and a designated team leader coordinating care during critical situations.
Roles and Responsibilities within the Team
PALS resuscitation teams require defined roles for optimal function, as outlined in the PALS PDF. The team leader manages the resuscitation, directing compressions, airway, and medications.
A compressor delivers high-quality chest compressions, while the airway manager secures and maintains a patent airway. A medication provider prepares and administers drugs accurately.
A scribe meticulously records events, interventions, and vital signs, ensuring a clear timeline. Additional members may assist with monitoring, family communication, and equipment retrieval, all vital for successful pediatric resuscitation.
Effective Team Communication
PALS emphasizes clear, concise communication for successful resuscitation, detailed within the PALS PDF. Closed-loop communication—order, confirmation, action—minimizes errors and ensures understanding.
Standardized terminology and a respectful tone foster collaboration. Briefings before scenarios clarify roles and expectations, promoting proactive teamwork.
Regular debriefings after events allow for constructive feedback and improvement. Active listening, avoiding interruptions, and clear articulation are crucial for optimal team performance during critical pediatric emergencies.
Team Leader Responsibilities
The PALS team leader, as detailed in the PALS PDF, directs resuscitation efforts, ensuring systematic assessment and intervention. They delegate tasks clearly, monitor progress, and maintain situational awareness.
Effective leaders facilitate open communication, encourage input from team members, and resolve conflicts promptly. They synthesize information, make informed decisions, and adapt the plan as needed.
Ultimately, the leader’s role is to optimize team performance, ensuring the best possible outcome for the pediatric patient during a critical emergency situation.

PALS Algorithms
PALS utilizes structured algorithms – bradycardia, tachycardia, and respiratory failure – detailed in the PALS PDF, guiding systematic assessment and treatment.
These algorithms provide a clear, step-by-step approach to pediatric resuscitation, ensuring consistent and effective care during emergencies.
Bradycardia Algorithm
The Bradycardia Algorithm, detailed within the PALS PDF, provides a systematic approach to managing slow heart rates in pediatric patients. Initial steps involve assessing the patient, providing ventilation support, and establishing intravenous access.
If bradycardia persists despite adequate ventilation, the algorithm guides interventions like epinephrine administration. Further steps include considering atropine and, ultimately, pacing if necessary. The PALS algorithm emphasizes continuous monitoring and reassessment throughout the process, adapting treatment based on the child’s response and clinical condition.
Tachycardia Algorithm
The Tachycardia Algorithm, comprehensively outlined in the PALS PDF, guides the management of fast heart rates in pediatric emergencies. Initial assessment focuses on determining if the tachycardia is compensated or decompensated, influencing immediate actions.
For unstable patients, synchronized cardioversion is indicated. Stable tachycardia management involves vagal maneuvers and, if ineffective, adenosine administration. Further steps may include amiodarone, guided by the PALS protocol, with continuous monitoring and reassessment crucial for adapting treatment.
Respiratory Failure Algorithm
The Respiratory Failure Algorithm, detailed within the PALS PDF, provides a systematic approach to managing pediatric respiratory distress. Initial steps involve assessing airway patency, breathing effectiveness, and circulation status, guiding immediate interventions.
Oxygenation and ventilation are prioritized, potentially requiring bag-mask ventilation or intubation. Addressing underlying causes is crucial, alongside continuous monitoring of oxygen saturation and carbon dioxide levels. The PALS protocol emphasizes prompt recognition and intervention to prevent further deterioration.
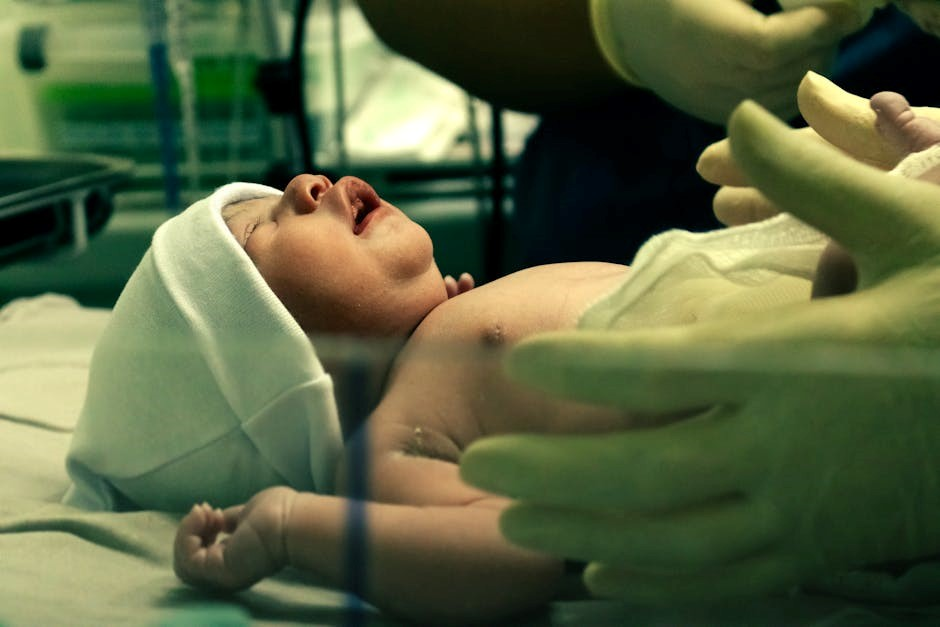
Cardiopulmonary Resuscitation (CPR) in Pediatrics
Pediatric CPR techniques, detailed in the PALS PDF, differ from adult CPR, emphasizing appropriate compression depth and rate for infants and children.
Effective airway management and ventilation are critical components, alongside early defibrillation when indicated, per PALS guidelines.
CPR Techniques for Infants
Infant CPR, as detailed within the PALS Provider Manual PDF, requires specific modifications compared to adult techniques. Chest compressions should be delivered using two fingers, positioned just below the nipple line, depressing the chest approximately 1.5 inches.
A compression-to-ventilation ratio of 30:2 is recommended for single rescuers, while two rescuers should maintain a ratio of 15:2. Effective airway management involves gentle head tilt-chin lift maneuvers, avoiding overextension. The PALS course emphasizes proper technique to maximize circulatory support and oxygenation during resuscitation efforts.
CPR Techniques for Children
Child CPR, as outlined in the PALS Provider Manual PDF, differs from infant CPR due to anatomical variations. Healthcare providers should utilize the heel of one or two hands for chest compressions, aiming for a depth of approximately 2 inches.
Maintaining a compression-to-ventilation ratio of 30:2 for single rescuers and 15:2 for two rescuers is crucial. Proper airway management involves a head tilt-chin lift, ensuring an open airway. The PALS course stresses the importance of adapting CPR techniques based on the child’s size and age.
Airway Management During CPR
Effective airway management during pediatric CPR, detailed in the PALS Provider Manual PDF, is paramount for successful resuscitation. Techniques include the head-tilt/chin-lift maneuver, carefully avoiding excessive extension, and jaw-thrust if spinal injury is suspected.
Oropharyngeal airways (OPAs) and nasopharyngeal airways (NPAs) may be utilized, with appropriate sizing crucial. The PALS course emphasizes prompt recognition and management of airway obstruction, including foreign body removal, ensuring optimal oxygenation and ventilation throughout the resuscitation process.
Pharmacological Management in PALS
PALS utilizes medications like epinephrine and amiodarone, detailed in the PALS Provider Manual PDF, for specific rhythms and conditions during pediatric resuscitation efforts.
Epinephrine Administration
Epinephrine is a cornerstone drug in PALS, crucial for increasing heart rate and blood pressure during cardiac arrest and severe bradycardia, as detailed in the PALS Provider Manual PDF.
The recommended dose varies based on weight and clinical scenario; intravenous (IV) or intraosseous (IO) routes are preferred, with careful consideration of concentration and potential side effects.
PALS guidelines emphasize prompt administration and continuous monitoring, ensuring appropriate response and minimizing adverse reactions, all thoroughly covered within the comprehensive manual.
Amiodarone Usage
Amiodarone serves as an antiarrhythmic agent in PALS, specifically indicated for refractory ventricular fibrillation or pulseless ventricular tachycardia unresponsive to defibrillation and epinephrine, as outlined in the PALS Provider Manual PDF.
Dosage is weight-based, administered intravenously over several minutes, demanding careful monitoring for hypotension and other adverse effects. It’s not a first-line drug but vital in specific cases.
PALS protocols emphasize cautious use and continuous assessment, ensuring benefits outweigh risks, comprehensively detailed within the official training materials and PALS PDF resource.
Other Essential Medications
Beyond epinephrine and amiodarone, PALS utilizes several crucial medications, detailed within the PALS Provider Manual PDF. These include sodium bicarbonate for specific cases of bradycardia and potential metabolic acidosis, as indicated by guidelines.
Glucose is vital for hypoglycemia, while naloxone reverses opioid-induced respiratory depression. Understanding appropriate dosages and administration routes is paramount, as emphasized in PALS training.
The PALS PDF resource provides comprehensive pharmacological information, ensuring providers are prepared to manage diverse pediatric emergencies effectively and safely.
Post-Resuscitation Care
Post-Resuscitation Care, detailed in the PALS PDF, focuses on stabilization, monitoring vital signs, temperature management, and thorough neurological assessments for optimal recovery.
Monitoring and Stabilization
Monitoring and Stabilization, as comprehensively covered within the PALS PDF, are paramount following successful resuscitation. Continuous assessment of vital signs – heart rate, respiratory rate, blood pressure, and oxygen saturation – is crucial.
Establish intravenous access for medication administration and fluid resuscitation. Closely monitor cardiac rhythm for any recurrence of instability. Address underlying causes contributing to the initial arrest, ensuring appropriate interventions are implemented to prevent further deterioration.
Maintain airway patency and provide adequate ventilation, adjusting support as needed based on the child’s clinical status.
Temperature Management
Temperature Management, detailed in the PALS PDF, is a critical component of post-cardiac arrest care. Both hypothermia and hyperthermia can negatively impact neurological outcomes in pediatric patients.
Actively prevent hypothermia by utilizing warming blankets, warmed intravenous fluids, and maintaining a warm environment. Monitor core temperature continuously. Avoid shivering, as it increases metabolic demand.
If hyperthermia is present, initiate cooling measures, recognizing that fever can exacerbate neurological injury. Prompt temperature control optimizes recovery.
Neurological Assessment
Neurological Assessment, thoroughly covered in the PALS PDF, is paramount post-resuscitation to evaluate for potential brain injury. This involves assessing level of consciousness using tools like the Pediatric Glasgow Coma Scale (PGCS).
Pupillary response, motor function, and reflexes should be frequently monitored. Look for signs of seizure activity. Serial assessments are crucial to detect subtle changes indicating neurological deterioration.
Early identification of neurological compromise guides further management and prognostication, optimizing long-term outcomes for the pediatric patient.

Specific Pediatric Emergencies
PALS PDF resources detail managing common emergencies like respiratory distress, shock, and seizures in pediatric patients, offering algorithm-based guidance.
Effective care requires rapid assessment and tailored interventions based on the child’s specific condition.
Respiratory Distress
The PALS PDF comprehensively covers respiratory distress, a frequent pediatric emergency requiring swift intervention. Assessment focuses on recognizing signs like increased work of breathing, altered mental status, and abnormal lung sounds.
Management strategies detailed within the manual include oxygen therapy, assisted ventilation techniques (like bag-valve-mask), and potential medication administration. PALS algorithms guide providers through systematic evaluation and treatment, emphasizing early recognition and stabilization of the airway, breathing, and circulation. Understanding underlying causes, such as asthma or bronchiolitis, is crucial for effective care.
Shock
The PALS PDF dedicates significant attention to pediatric shock, a life-threatening condition demanding rapid recognition and intervention. The manual details differentiating hypovolemic, cardiogenic, and distributive shock, crucial for targeted treatment.
PALS algorithms guide providers through fluid resuscitation, vasoactive medication administration, and addressing the underlying cause. Assessment includes evaluating perfusion – heart rate, blood pressure, capillary refill – and mental status. Early intervention, as outlined in the PALS course, is paramount to prevent progression to irreversible organ damage.
Seizures
The PALS PDF comprehensively covers pediatric seizure management, emphasizing rapid assessment and intervention. It details differentiating seizure types – febrile, provoked, unprovoked – guiding appropriate treatment strategies. PALS algorithms outline steps for terminating prolonged seizures, including benzodiazepine administration.
The manual stresses airway management, oxygenation, and monitoring vital signs during and after seizure activity. Identifying underlying causes, like infection or metabolic disturbances, is crucial. PALS training, detailed in the PDF, prepares providers for effective seizure care.

Additional Tools and Resources
PALS offers reference cards and online resources to reinforce learning from the PDF manual. Practice questions and exam preparation materials are also available.
PALS Reference Cards
PALS Reference Cards are laminated, full-color guides included with the PALS Provider Manual, offering quick access to essential algorithms and drug dosages during critical situations.
These cards serve as invaluable tools for rapid recall of vital information, streamlining decision-making in fast-paced pediatric emergencies. They condense complex protocols into easily digestible formats.
The PALS PDF manual complements these cards, providing detailed explanations, while the cards facilitate immediate application of knowledge during resuscitation efforts, enhancing patient outcomes.
Online PALS Resources
Numerous online PALS resources supplement the PALS Provider Manual and course, offering digital access to algorithms, practice questions, and updated guidelines from the American Heart Association.
These platforms often include interactive modules and video demonstrations, reinforcing key concepts presented in the PALS PDF. They provide a flexible learning environment for review and skill enhancement.
Accessing these digital tools allows healthcare professionals to stay current with the latest ECC guidelines and refine their pediatric resuscitation skills, improving patient care quality.
Practice Questions and Exam Preparation
Effective PALS exam preparation relies heavily on utilizing practice questions mirroring the format and content of the actual assessment, often found alongside the PALS PDF.
These questions assess comprehension of algorithms, pharmacological interventions, and BLS/ALS integration, crucial for successful course completion and certification.
Reviewing a comprehensive study guide with 700+ practice questions, as some resources offer, significantly boosts confidence and identifies areas needing further study before the PALS exam.

American Heart Association Guidelines
PALS courses directly reflect the latest AHA guidelines for CPR and emergency cardiovascular care, updated regularly and detailed within the PALS PDF.
PALS Course Reflects AHA Guidelines
Pediatric Advanced Life Support (PALS) training is fundamentally built upon the science and educational principles established by the American Heart Association (AHA). The course content meticulously aligns with the most current AHA Guidelines Update for Cardiopulmonary Resuscitation (CPR) and Emergency Cardiovascular Care (ECC).
These guidelines, comprehensively documented within the PALS Provider Manual and accessible in PALS PDF formats, ensure healthcare professionals receive evidence-based instruction. Regular updates to these guidelines are seamlessly integrated into the PALS curriculum, guaranteeing providers are equipped with the latest best practices for pediatric emergency care.
Updates to ECC Guidelines
The American Heart Association (AHA) continuously refines its Emergency Cardiovascular Care (ECC) guidelines based on the latest scientific evidence and resuscitation research. These crucial updates are promptly incorporated into the Pediatric Advanced Life Support (PALS) course curriculum, ensuring providers receive the most current, effective techniques.
Accessing the updated PALS Provider Manual or a current PALS PDF resource is vital for staying informed. Changes often involve refinements to algorithms, pharmacological recommendations, and BLS/CPR protocols, all designed to improve pediatric resuscitation outcomes.
Importance of Staying Current
Pediatric resuscitation practices evolve rapidly with new research and advancements in care. Regularly updating your PALS knowledge is therefore paramount for providing optimal patient outcomes. Relying on outdated information from an older PALS PDF can compromise a child’s life during a critical event.
Consistent review of the latest AHA guidelines, through the PALS Provider Manual or updated digital resources, ensures proficiency. Staying current demonstrates a commitment to best practices and enhances confidence in managing pediatric emergencies effectively.

PALS Pre-Course Assessment
The PALS Pre-Course Assessment, found within the PALS PDF, evaluates existing knowledge and identifies areas needing focus before the course begins.
It covers essential concepts, preparing learners for the intensive PALS training and maximizing the learning experience.
Purpose of the Pre-Course Assessment
The primary goal of the PALS Pre-Course Assessment, readily available within the comprehensive PALS PDF manual, is to gauge a participant’s existing foundational knowledge of pediatric advanced life support principles.
This assessment isn’t designed to be a pass/fail evaluation, but rather a self-assessment tool. It helps identify knowledge gaps and areas where focused review will be most beneficial before engaging in the intensive course content.
By completing it, individuals can proactively prepare, ensuring a more effective and rewarding learning experience during the PALS provider course itself.
Areas Covered in the Assessment
The PALS Pre-Course Assessment, detailed within the PALS PDF manual, comprehensively evaluates core competencies essential for effective pediatric resuscitation. Key areas include basic life support (BLS) skills for infants and children, recognizing and managing bradycardia and tachycardia.
It also assesses understanding of respiratory emergencies, shock, and the initial steps in managing various pediatric illnesses. Furthermore, the assessment touches upon pharmacological interventions and post-cardiac arrest care principles.
Successfully navigating these topics demonstrates preparedness for the full PALS course.
Preparing for the PALS Course
Effective preparation for the PALS course begins with thoroughly reviewing the PALS Provider Manual PDF. Familiarize yourself with the algorithms for bradycardia, tachycardia, and respiratory failure, practicing their application through case studies.
Complete the pre-course assessment to identify knowledge gaps and focus your study efforts. Brush up on basic life support (BLS) skills, ensuring proficiency in infant and child CPR techniques.
A solid foundation will maximize your learning experience.




